Nurses share their stories...
Whanau and families have described them... special and dedicated people.
We have had comments of ... "The overall care in such a fragile situation was always respectful, thoughtful, and compassionate"
Our nēhi or nurses - reluctantly share their very sensitive stories...they are working throughout Taranaki, and they love their job.
In this series, they share how passionately they feel about the specialised work of a palliative care nurse and the importance of teamwork that in turn supports them. They highly recommend the job to other nurses. We are exceptionally proud of them.
(Nurses' stories transcribed by Lyn Humphries)
Introducing Sharon (July 2023)
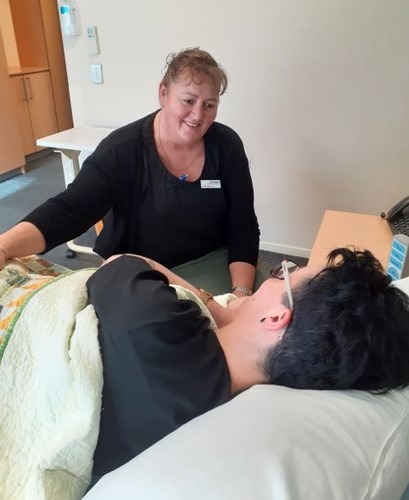
Sharon Campbell is deeply passionate about the hands-on holistic care she and her fellow nurses can offer hospice patients whose end is near.
“We can make a difference,” says Sharon, Taranaki hospice’s community team leader.
Sharon graduated as a nurse in 1983 when she was among the last to go through hospital-based training in New Plymouth. After seeing the value of palliative care nursing while working in rest homes, she has now spent 11 ½ years caring for the dying.

“People say to me it’s a bit gloomy caring for the dying but I believe it’s actually a privilege to support people at the end of their life."
The job is very community-focussed with support the key. “A loved one can’t do it on their own.” There is a wide variety of support and advice they can offer to people who might never have been in the position of knowing what was ahead and no idea what may be available to them. Nurses often make referrals on their behalf to other helpful community-based support services.
“Our aim is to keep them at home if that’s where they want to be. We will do anything to support people at home if that is their wish.”
Some relationships between nurse and patient could be many months long during which time it is inevitable that they become close and personal. “We spend a lot of time with some patients. We get close to them and chat with them about the little things. It helps puts things in the real world for them.
“One particular lady was tripping away,” Sharon recalls fondly. She had enjoyed many trips overseas during her lifetime. “Her joy came from listening to our discussions about our own voyages.”
Another recent example was the close bond that developed between herself and the colourful New Plymouth photojournalist Rob Tucker* and his family. Sharon says Rob gave her many a laugh sharing hilarious tales of his adventures on the job. Sipping Queen Elizabeth II’s gin when she left the room was a favourite.
“I had him on about that one! He could tell some really good stories.” Rob died recently but not until organizing a massive fundraising effort for the hospice coffers through an auction of famous photos he talked his mates into handing over. They raised nearly $200,000, the most successful fundraiser ever for Te Kahu Pairuri Hospice Taranaki.
The law The End of Life Choice Act which legalised euthanasia for a small number of terminally ill people from November 7 2021, is now another option for those who might qualify to end their lives through medical intervention. “We do get asked about it, Sharon says. “If that is what they want, we still continue to support them. That was a challenge (when the law was passed). We all have individual thoughts on it. But it is the patient’s choice and we accept that. It is an entirely individualized choice.”
The hospice works hard to keep up to date. “As the hospice has moved forward, changes have been made to the referral process,” Sharon says. The focus is always on what the patients themselves want and this is reviewed on a regular basis. Some patients may even be temporarily discharged.
The Taranaki hospice is a rarity in that it offers 24/7 care to its patients throughout the region. Most nurses work on a morning shift travelling around the region to see their home-based patients. One person is rostered to be on-call during the night. “Very few other hospices give overnight care these days,” Sharon says.
The hospice nurses are well loved by a grateful Taranaki community. There is good reason they are called the Hospice Angels for the exceptional care they offer at a time which can be the most stressful in a family’s life. But while she highly commends the work, it is not for everyone, Sharon warns.
“I do think it’s a calling. In a lot of nursing you are dealing with one issue. On the one hand, palliative care nurses are getting to know their patient well - right through to the end of their life. “And there is nothing more rewarding than that.” And then there is the indisputable truth that you are born and you will die, she says. “I think it has taught me that you don’t sweat the small stuff.” It helps put both work and home into perspective and to value life every day.
The family support is not over when their loved one dies, Sharon points out. And nurses also value the bereavement care through checking in with the families. “It’s really important, as well as for the nurse. We call in and have a chat and a cuppa, make sure people are eating, sleeping and have support around them." They can also be referred to a support group and receive counselling. And it’s all free.
Nurses themselves can also receive support after the death of their patient both through the camaraderie of other nurses and take advantage of clinical supervision.
De-stressing from the intensity of the job she deals with through her love of nature, her dogs, birds and garden.
“I find having a coffee sitting on the deck and watching the birds does it for me. I just switch off.”
Now aged 62, having raised three children and with two grandchildren, Sharon has no intention of giving the job away. Even though close to retirement age, she can see herself cutting back a bit while still continuing in the role.
“I still love getting up in the morning and coming to work. And also to work with great staff.”
* Rob's name included with the family's permission.
Introducing Marie (July 2023)
In the early 2000s, Marie Appert was one of the youngest nurses at that time to take up palliative care nursing. She was in her late 20s and a young mum.
“I was working in a rest home and hospital as well and my plan was to do midwifery but my plans changed after having my children. I applied for the hospice job when my children were quite young. Twenty years later and I haven’t wanted to work anywhere else. That shows how much I love it.”
Marie lives and farms with her husband about a 20km drive from the hospice. She takes that time to unwind and turn her focus on her own full-on life.
To Marie, the inevitable journey towards death has now been well and truly put in perspective.
“I am quite resilient in caring for patients as their quality of life reduces. Everyone’s journey is quite unique. Some fight every step and some are more accepting.
“We can tell them it’s okay to go and that their loved ones who are left behind will be supportive of their decision and will be okay.”
While most of their palliative care patients have led a full life, the toughest to care for will always be the youngsters and supporting their parents who are experiencing the reversal of the norm in losing their child before them.
“I have looked after many children. It is the parents needing support, knowing their child is not supposed to go first.”
Hospice nurses have inevitably experienced personal losses of loved ones. “I have looked after family at the end whom I have cared for. So we nurses have that empathy, that understanding.
“I think because of my job, I look at life very differently because you never know what’s around that corner and you value your family and your friends.”
Death of a loved one can bring out strong emotions and it is not unknown for them to take out their frustration on the nurses. “Sometimes they take it out on you. We see the good, the bad and the ugly but you can’t take anything personally. Apologies invariably follow the angry outbursts. At the end, it’s part of acceptance.”
Marie is now 51 and a grandmother and she has lost count of the number of patients she has cared for over the years. It is not unknown for people to see her out and about and introduce her as the nurse that cared for their loved one. “At first I don’t always remember them but as soon as we start talking it all comes back.”
And over those two decades she has experienced a dramatic change in palliative care. “There is lots of variety in the work. While in the past, palliative patients were mostly cancer-related now there is a 50-50 mix of cancer and medical cases such as heart, motor neurone disease and lung disease". As a result, Marie advises nurses to get solid experience before joining palliative nursing.
“Hospice is an amazing place to work. It is a great team, we definitely support each other. Hospice becomes your family. You need each other to survive in this line of work. A lot of things you learn as you go and things are changing all the time. There is now a lot more treatment available. People are now living longer. Some people get treatment right until they die now. Some people are cared for just for days to weeks, others are months to years. Some are even discharged. You get a real variety.
“There are many more treatment options and trials these days. Some people cling to anything and give anything a go. And sometimes they have no quality of life at all.”
As a consequence, she now has her own philosophy on what she would do put in the same position and suggests it is important to look at the big picture.
“I have very clear views, if it was me in the same position, how I would want to be treated. I’m here for a good time not a long time is my philosophy. Quality of life is the most important.”
Marie acknowledges that caring for the dying and supporting their loved ones is not for everyone. Adaptability is an essential skill.
“It is not everyone’s job, that’s for sure. You can’t run to a timetable. You can’t schedule appointments. You just never know. You have to be easy-going. Sometimes you are getting up in the middle of the night and can be anywhere at any time. I can sleep any time, anywhere and get up and go any time.” There were times her husband never realized she had been up on call at night and back in bed again before he woke up.
Knowing how fragile life can be, Marie urges her own family and friends to ensure they have plans in place for the unexpected and inevitable.
One of the best tools to assist in doing this is completing an Advance Care Planning booklet, she says, which many are unaware even exists. Palliative care patients are offered it through hospice.
Marie is now looking forward to a new challenge in her career as the inpatient unit team leader. “It’s exciting. We have new staff come on board in the last couple of years.” She is looking forward to helping guide and train the newcomers and pass on her knowledge.
It is not unknown for some nurses to leave, then realize how much they valued the job and the team and have returned.
“But if you are not a team player you won’t fit in,” she warns. “You can’t do this on your own. I just utterly enjoy my job and the hospice family I work with.”
“Anyone interested should come in and talk to one of us.”
